1.800.858.7378npic@oregonstate.edu
Call, email, or chat Mon-Fri
A to Z
Medical Case Profile: Inhalation Risks from Phosphide Fumigants
Inhalation Risks from Phosphide Fumigants
Medical Cases and Topics for Health Care Providers are based upon inquiries received by NPIC, as well as relevant publications in the scientific literature. They are intended to educate health care providers about pesticide toxicology.
Scenario:
A 48 year old male acutely develops symptoms of chest pain, shortness of breath, dizziness, and nausea with an episode of vomiting. The symptoms develop acutely at the workplace, where he is employed as a production worker at an aluminum phosphide manufacturing facility. He is brought to the company physician and is noted to be alert and responsive with a normal respiratory rate, but appearing pale, sweaty, and acutely ill. He has no prior history of heart disease, and a recent exercise stress test that was normal. On initial examination, the heart rate is slow with distant heart sounds. The initial blood pressure is 78/58, and a rhythm strip indicates a junctional bradycardia (rate 58). He is transported via ambulance to an emergency room, with suspicion that he is having a myocardial infarction.
An initial ECG shows normal sinus rhythm with non-specific ST and T-wave abnormalities. Laboratory analyses reveal an elevated creatine phosphokinase (CK 247 U/L), with a normal CK-MB index and a normal troponin I. Other laboratory values, including tests of renal and liver function, are within normal limits. Serum magnesium is not measured. He is admitted to the hospital with a diagnosis of acute chest pain, to rule out unstable angina. Over the next six hours, his symptoms resolve. He does not develop arrhythmias or other clinical or laboratory signs of cardiac injury, and discharged from the hospital the next day.
Discussion:
This case demonstrates the importance of an occupational exposure history, because in some cases the signs and symptoms of an acute occupational pesticide exposure can be life-threatening. The identification of occupational risk factors can lead to opportunities to prevent unnecessary exposure. In this case, the worker’s occupation involved rotation through several different steps in the manufacturing process of aluminum phosphide. Further history taking identified safety concerns including air filters that frequently became clogged with dust generated through the manufacturing process, and poor compliance with the use of required respiratory protective gear. The worker also described previous episodes in which co-workers involved in the manufacturing process became acutely ill while performing routine tasks. A review of the chemistry and toxicology of aluminum phosphide identifies reasons that the health care provider should recognize this class of occupational and environmental hazards.
Aluminum phosphide is a pesticide registered in the United States for the indoor fumigation of agricultural commodities, animal feeds, processed foods, and structural as well as outdoor pest control. The chemical is usually formulated in pellets, granules, or as a dust. Upon contact with moisture in the environment, aluminum phosphide undergoes a chemical reaction yielding phosphine gas which is the active pesticidal component (Figure 1). In addition to these chemical properties, phosphine may spontaneously ignite in the presence of oxygen at concentrations above a threshold limit range of .48-1.9% (v/v).1
Figure 1: Aluminum phosphide and liberation of phosphine gas
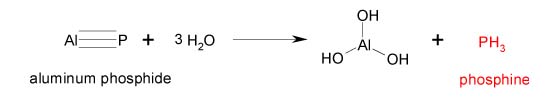
Phosphine, a nucleophile which acts as a strong reducing agent, is capable of interacting with and inhibiting cellular enzymes involved in metabolic processes. Early studies of phosphine demonstrated specific inhibitory effects on mitochondrial cytochrome c oxidase.2 Experimental and observational studies have subsequently demonstrated that the inhibition of cytochrome c oxidase and other enzymes leads to the generation of superoxide radicals and cellular peroxides. Cellular injury subsequently occurs through lipid peroxidation and other oxidant mechanisms.3,4 The four hour inhalation LC50 of phosphine gas has been measured to be 11 ppm (approximately 0.014 mg/L) in animal (rat) studies, which places it in the highest toxicity category (U.S. EPA signal word "Danger") for acute inhalation exposure.5
Overexposure to phosphine from aluminum phosphide can result in the rapid onset of gastrointestinal signs and symptoms including nausea, epigastric pain and vomiting.6 Cardiovascular manifestations of acute overexposure to phosphine include hypotension and bradycardia.6 Non-specific ST-T wave changes on the electrocardiogram have been frequently reported, as well as left ventricular systolic dysfunction on the echocardiogram.7 Myocardial and skeletal muscle injury can occur.8 Increased CK with a normal CK-MB fraction has been reported in association with acute overexposure to phosphine in a workplace.9 Pulmonary injury and edema have been described after inhalation exposure.10 Neurological manifestations following acute exposure include headache and dizziness, which frequently occur in the presence of a normal mental state.6,11 Acute renal and liver injury can also develop in cases of severe intoxication.7,12
Very little information is available relating to the toxicokinetics of phosphine in humans. In an investigation of a series of patients with intoxication from aluminum phosphide, indicators of oxidative stress appeared to peak within 48 hours of exposure, with normalization of most indicators occurring by day 5.4 Reliable biomarkers of exposure to phosphine are not readily available.13 The management of acute intoxication from phosphine inhalation is primarily supportive. Hypomagnesemia is a frequent complication of acute intoxication from phosphine gas exposure.14 The administration of intravenous magnesium has been associated with significant improvement in indicators of oxidative stress (malonyldialdehye, reduced glutathione) and a lower incidence of mortality (20%) in comparison to control subjects (44% mortality) in cases of severe phosphine intoxication.15 In the current case an investigation of phosphine gas levels was not conducted on the date that the worker became symptomatic, making it difficult to conclusively determine that inhalation exposure was responsible. The signs and symptoms that were experienced were consistent with overexposure to phosphine gas. Although phosphine gas is reported to have a characteristic fishy odor, and this odor has been suggested to be a potential warning sign indicating an unacceptable level of inhalation exposure, it has been observed that many individuals may not be able to detect this odor at levels that may pose risks of adverse effects.11 A Permissible Exposure Limit (PEL) of 0.3 ppm (as an eight hour, time-weighted average) has been established for phosphine gas in the workplace by the Occupational Safety and Health Administration. The National Institute of Occupational Safety and Health considers levels of phosphine greater than 50 ppm to be Immediately Dangerous to Life and Health (IDLH).
The National Institute of Occupational Safety and Health has developed a series of recommendations for the protection of workers who may be exposed to phosphine gas during fumigations, which emphasize the importance of worker education, air monitoring, and engineering controls as the most important methods to reduce unnecessary exposure.11 NIOSH also provides additional recommendations for the use of respiratory protection for workers with exposure to phosphine gas in the workplace. Fumigants containing aluminum and magnesium phosphide as active ingredients have gone through the reregistration process by the U.S. Environmental Protection Agency. Based upon a review of the available toxicology data, the EPA has required changes in the use of phosphide fumigants, which are intended to minimize the risk to workers handling these pesticides as well as bystanders in the vicinity of applications. As the risks of major morbidity and mortality are significant from exposure to phosphine gas, health care providers should be aware of these changes that impact workplace safety and recognize the potential hazards associated with phosphide fumigants.
References:
- Kondo S, Tokuhashi K, Nagai H et al. Spontaneous Ignition Limits of Silane and Phosphine. Combustion and Flame. 1995; 101:170.
- Chefurka W, Kashi KP, Bond EJ. The Effect of Phosphine [Gas Toxic to Insects] on Electron Transport in Mitochondria. Pestic Biochem Physiol. 1976; 6:65-84.
- Bolter CJ, Chefurka W. Extramitochondrial release of hydrogen peroxide from insect and mouse liver mitochondria using the respiratory inhibitors phosphine, myxothiazol, and antimycin and spectral analysis of inhibited cytochromes. Arch Biochem Biophys. 1990; 278:65-72.
- Chugh SN, Arora V, Sharma A et al. Free radical scavengers & lipid peroxidation in acute aluminium phosphide poisoning. Indian J Med Res. 1996; 104:190-193.
- United States Environmental Protection Agency, Office of Prevention Pesticides and Toxic Substances. Reregistration Eligibility Decision: Aluminum and Magnesium Phosphide. 1998.
- Gupta S, Ahlawat SK. Aluminum phosphide poisoning--a review. Journal of toxicology Clinical toxicology. 1995; 33:19-24.
- Gupta MS, Malik A, Sharma VK. Cardiovascular manifestations in aluminium phosphide poisoning with special reference to echocardiographic changes. The Journal of the Association of Physicians of India. 1995; 43:773-780.
- Khosla SN, Nand N, Kumar P et al. Muscle involvement in aluminium phosphide poisoning. The Journal of the Association of Physicians of India. 1988; 36:289-290.
- Dueñas A, Pérez-Castrillon JL, Cobos MA et al. Treatment of the cardiovascular manifestations of phosphine poisoning with trimetazidine, a new antiischemic drug. The American journal of emergency medicine. 1999; 17:219-220.
- Willers-Russo LJ. Three fatalities involving phosphine gas, produced as a result of methamphetamine manufacturing. Journal of forensic sciences. 1999; 44:647-652.
- National Institute of Occupational Safety and Health. NIOSH Alert: Preventing Phosphine Poisoning and Explosions During Fumigation. 99-126, 1-16. 2003. Columbus, Ohio. Accessible at: https://www.cdc.gov/niosh/docs/99-126/
- Arora B, Punia RS, Kalra R et al. Histopathological changes in aluminium phosphide poisoning. Journal of the Indian Medical Association. 1995; 93:380-381.
- Singh S. Serial blood phosphine levels in aluminium phosphide [ALP] poisoning. The Journal of the Association of Physicians of India. 1996; 44:841-842.
- Chugh SN, Kamar P, Sharma A et al. Magnesium status and parenteral magnesium sulphate therapy in acute aluminum phosphide intoxication. Magnes Res. 1994; 7:289-294.
- Chugh SN, Kolley T, Kakkar R et al. A critical evaluation of anti-peroxidant effect of intravenous magnesium in acute aluminium phosphide poisoning. Magnesium research : official organ of the International Society for the Development of Research on Magnesium. 1997; 10:225-230.
If you have questions about this, or any pesticide-related topic, please call NPIC at 800-858-7378, or email us at npic@oregonstate.edu.
